Many common prescription and over-the-counter drugs list dry eye as a known side effect, and for patients who already tend toward dryness, the impact can be significant. If your eyes have been feeling gritty, burning, or unusually sensitive since starting a new medication, you’re likely not imagining it.
The tricky part is that medication-induced dry eye often goes unrecognized. Patients assume their symptoms are seasonal, related to screen time, or just part of getting older. In reality, a pill they take every morning could be quietly reducing tear production or changing the makeup of their tear film.
Keep reading to learn which drug categories most commonly contribute to dry eye side effects, why they affect your eyes the way they do, and how an eye doctor can help you manage symptoms without abandoning the medications you need.
How Medications Affect Your Tear Film

To understand why certain drugs cause dry eye, it helps to know how tears work.
A healthy tear film has three layers: an oily outer layer produced by the meibomian glands in your eyelids, a watery middle layer from the lacrimal glands, and an inner mucus layer that helps tears adhere to the eye’s surface.
Some drugs reduce the volume of tears your lacrimal glands produce. Others disrupt the oily layer, allowing tears to evaporate faster than normal. A third mechanism involves anticholinergic effects, where medications block the chemical signals that tell your tear glands to function. This last mechanism is particularly common and explains why such a wide variety of drugs, from allergy pills to antidepressants, can all produce the same uncomfortable outcome.
Which Medications Commonly Cause Dry Eye Side Effects?
The list of medications associated with dry eye is broader than most patients expect. These are some of the most frequently encountered categories.
Antihistamines and Decongestants
Allergy medications are among the top contributors to medication-related dry eye. Antihistamines reduce mucus and aqueous tear production, and can affect tear film stability. Decongestants compound the problem by causing vasoconstriction that reduces blood flow to the lacrimal system, further lowering tear output.
Because the symptoms of dry eye and allergies often overlap, it can be difficult to know which one is driving your discomfort without a professional evaluation.
Antidepressants and Anti-Anxiety Medications
Tricyclic antidepressants have well-known anticholinergic properties that reduce both aqueous and mucus tear secretions. Selective serotonin reuptake inhibitors do not share the same anticholinergic mechanism but have still been linked to dry eye symptoms through less-understood pathways. Anti-anxiety medications in the benzodiazepine class also contribute to dryness.
Blood Pressure Medications
Beta-blockers can reduce tear secretion by decreasing the protein content your lacrimal glands need to produce adequate tears. Thiazide diuretics, commonly prescribed for high blood pressure and heart failure, alter fluid balance in the body in ways that change tear composition and reduce production. Other blood pressure medications, including ACE inhibitors, are generally considered lower risk for dry eye, though individual responses vary.
Isotretinoin (Accutane)
This acne medication carries a significant dry eye risk because it targets the sebaceous glands throughout the body, including the meibomian glands in the eyelids. By shrinking those glands, isotretinoin can permanently reduce or eliminate the oil layer of the tear film. Unlike other medication side effects that resolve when the drug is stopped, meibomian gland damage from isotretinoin can be long-lasting. Patients prescribed this medication should discuss proactive eye monitoring with their doctor before and during treatment.
Hormonal Medications and Others
Birth control pills and hormone replacement therapy (HRT) can also contribute to dry eye side effects, particularly formulations that use estrogen alone. Over-the-counter and prescription sleep aids, medications for overactive bladder, antipsychotics, and higher doses of ibuprofen have also been associated with reduced tear production or changes in tear quality.
What You Can Do About Medication-Induced Dry Eye

Finding out that a necessary medication is contributing to dry eye can feel frustrating, but there are meaningful steps you and your care team can take.
Do not stop medications on your own. Many drugs linked to dry eye treat serious conditions where abrupt discontinuation can be harmful. Always consult the prescribing physician before making any changes to your regimen.
Instead, discuss whether a lower dose or an alternative within the same drug class might produce fewer ocular side effects. Switching from a first-generation antihistamine to a second-generation version, or transitioning from an oral antihistamine to a nasal spray formulation, can meaningfully reduce the impact on your eyes. Your primary care provider and your eye doctor can collaborate to find options that protect both your general health and your eye comfort.
In the meantime, lubricating eye drops (artificial tears) are a practical first-line approach, and preservative-free formulations are generally preferred if you need drops more than four times per day. Warm compresses, omega-3 supplementation, and staying well hydrated can also support tear film health.
For patients who want to reduce reliance on drops altogether, there are other ways to manage dry eye symptoms worth discussing with your eye doctor.
It is also worth examining your daily routine, since certain habits can quietly worsen dry eye and compound the effects of medication over time.
How Blaine Eye Clinic Evaluates Dry Eye
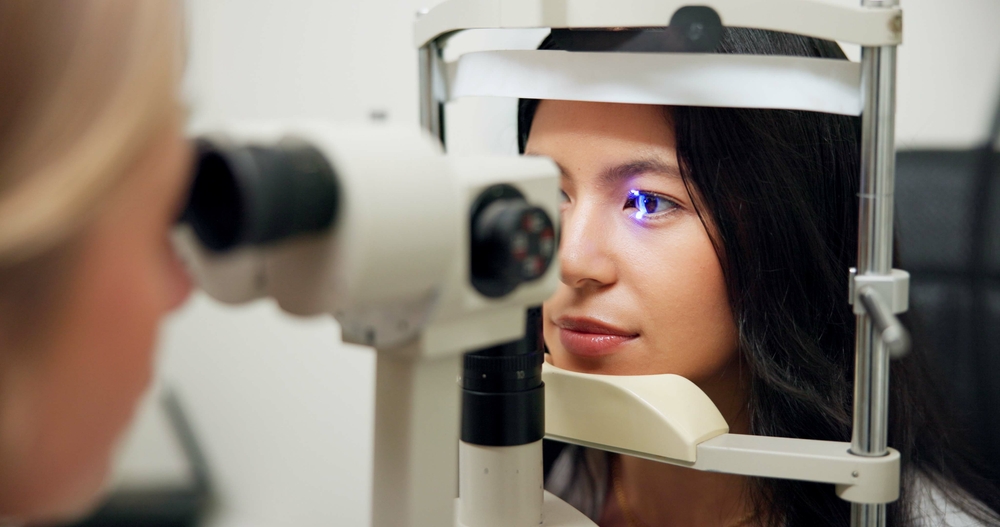
At Blaine Eye Clinic, dry eye evaluations go beyond asking if your eyes feel uncomfortable. When medication use is a potential factor, the team reviews your full medication list as part of the patient history and uses specialized diagnostic tools to get a clearer picture of what’s happening at the ocular surface.
TearLab osmolarity testing measures the salt concentration in your tears. Elevated osmolarity, known as hyperosmolarity, is a reliable indicator of tear instability and reduced tear quality.
InflammaDry detects elevated levels of MMP-9, an inflammatory marker frequently found in dry eye patients before other signs become visible.
In many cases, dry eye can be detected during a comprehensive eye exam before symptoms become severe, which is one of the strongest arguments for keeping up with annual visits even when your eyes feel fine.
If your eyes have been feeling different since a prescription change, that connection is worth exploring with a professional. Schedule a dry eye evaluation at Blaine Eye Clinic in Blaine, MN, today, and let our team help you find lasting relief!





